Quick Summary
- Procedure combining surgery with stem cell treatment promising for bulldog pups with spina bifida
- The pair of English bulldogs were the first dogs to receive the treatment
- Researchers hope to test the therapy in human clinical trials to help eradicate spina bifida in humans and dogs
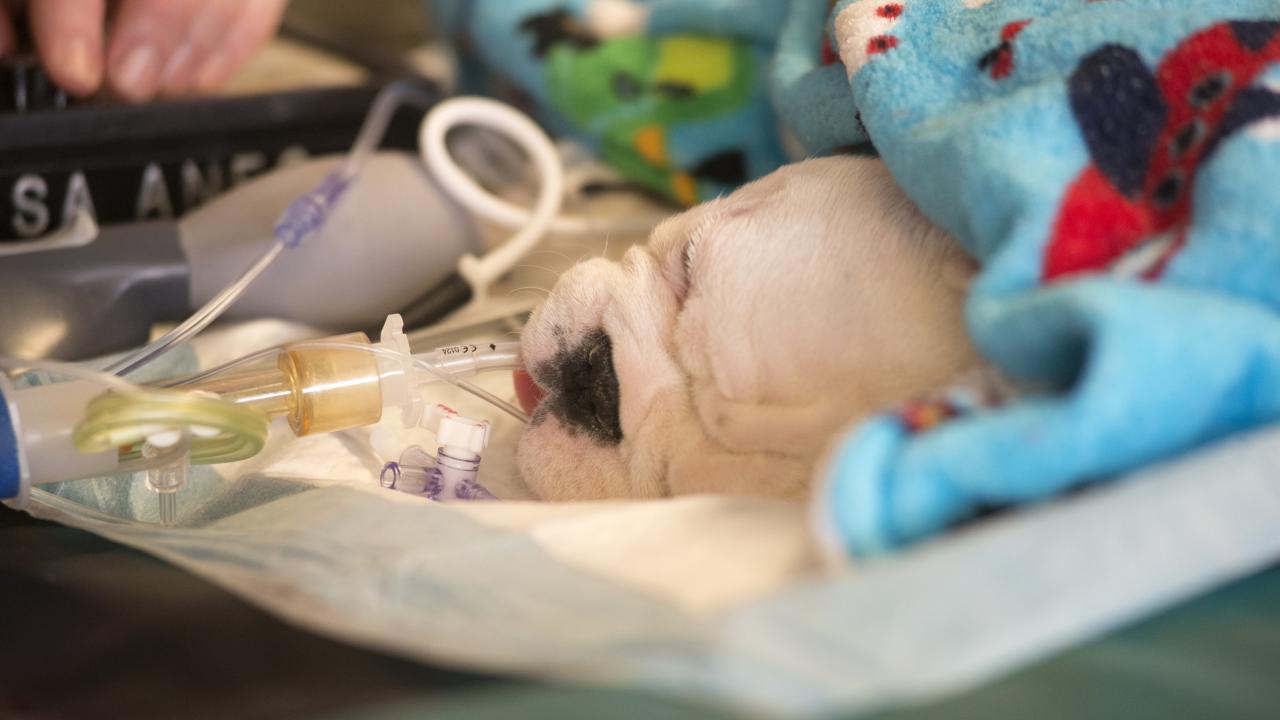
A pair of English bulldog puppies are the first patients to be successfully treated with a unique therapy — a combination of surgery and stem cells — developed at the University of California, Davis, to help preserve lower-limb function in children with spina bifida.
(Editor’s note: Photos and b-roll available.)
Because dogs with the birth defect frequently have little control of their hindquarters, they also have little hope for a future. They are typically euthanized as puppies.
At their postsurgery re-check at 4 months old, however, the siblings, named Darla and Spanky, showed off their abilities to walk, run and play to their doctor, veterinary neurosurgeon Beverly Sturges.
“The initial results of the surgery are promising, as far as hind limb control,” said Sturges. “Both dogs seemed to have improved range of motion and control of their limbs.”
The dogs have since been adopted, and continue to do well at their home in New Mexico.
A major step toward curing spina bifida
Spina bifida occurs when spinal tissue improperly fuses in utero, causing a range of cognitive, mobility, urinary and bowel disabilities in about 1,500 to 2,000 children born in the U.S. each year. The dogs’ procedure, which involved surgical techniques developed by fetal surgeon Diana Farmer of UC Davis Health together with a cellular treatment developed by stem cell scientists Aijun Wang and Dori Borjesson, director of the university’s Veterinary Institute for Regenerative Cures, represents a major step toward curing spina bifida for both humans and dogs.
Farmer pioneered the use of surgery prior to birth to improve brain development in children with spina bifida. She later showed that prenatal surgery combined with human placenta-derived mesenchymal stromal cells (PMSCs), held in place with a cellular scaffold, helped research lambs born with the disorder walk without noticeable disability.
Sturges wanted to find out if the surgery-plus-stem-cell approach could give dogs closer-to-normal lives along with better chances of survival and adoption. At 10-weeks old, Darla and Spanky were transported from Southern California Bulldog Rescue to the UC Davis veterinary hospital, where they were the first dogs to receive the treatment, this time using canine instead of human PMSCs.
Another distinction for Darla and Spanky is that their treatment occurred after birth, since prenatal diagnosis of spina bifida is not performed on dogs, Sturges explained. The disorder becomes apparent between 1 and 2 weeks of age, when puppies show hind-end weakness, poor muscle tone, incoordination and abnormal use of their tails.
A unique environment for collaborative research
UC Davis is the only place where this type of cross-disciplinary, transformational medicine could happen, according to Farmer.
“It’s rare to have a combination of excellent medical and veterinary schools and strong commitment to advancing stem cell science at one institution,” she said.
UC Davis is also home to the One Health initiative aimed at finding novel treatments like these for diseases that affect both humans and animals.
“I’ve often said that I have the greatest job on the planet, because I get to help kids,” Farmer said. “Now my job is even better, because I get to help puppies too.”
Hopes for clinical trials in humans and dogs
With additional evaluation and U.S. Food and Drug Administration approval, Farmer and Wang hope to test the therapy in human clinical trials. Sturges and Borjesson hope to do the same with a canine clinical trial. They hope the outcomes of their work help eradicate spina bifida in dogs and humans.
In the meantime, the team wants dog breeders to send more puppies with spina bifida to UC Davis for treatment and refinements that help the researchers fix an additional hallmark of spina bifida — incontinence. While Darla and Spanky are very mobile and doing well on their feet, they still require diapers.
“Further analysis of their progress will determine if the surgery improves their incontinence conditions,” Sturges said.
Funding for this project was provided by the Veterinary Institute for Regenerative Cures (VIRC) at the UC Davis School of Veterinary Medicine, and the Surgical Bioengineering Lab at the UC Davis School of Medicine. Private donations to the veterinary school for stem cell research also contributed to this procedure. Farmer and Wang’s spina bifida research is supported by funding from the National Institutes of Health, the California Institute for Regenerative Medicine, Shriners Hospitals for Children and the March of Dimes Foundation.
Media Resources
Kat Kerlin, UC Davis News and Media Relations, 530-750-9195, kekerlin@ucdavis.edu
Karen Finney, UC Davis Health, 916-734-9064, klfinney@ucdavis.edu